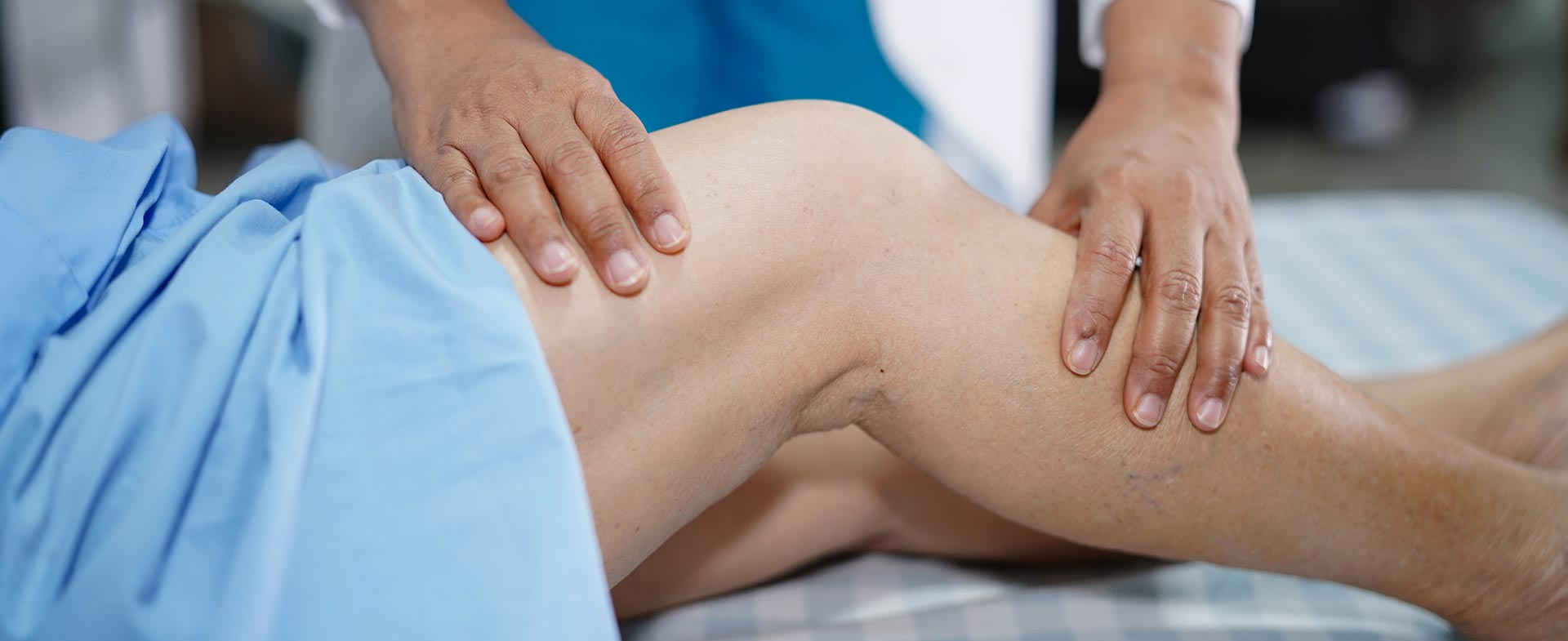
Varicose veins can be a real pain. But what causes them, and how can they be treated?
Henry Ford Health vascular surgeon Paul Corcoran, M.D., answers frequently asked questions about varicose veins.
The Inside Story On Veins
Varicose veins affect up to 35% of Americans. Dr. Corcoran discusses what lies beneath this common condition.
What are varicose veins?
“Varicose veins are twisted, bulging and enlarged veins that are visible beneath the surface of the skin,” says Dr. Corcoran. “Some people are bothered by their ropy, discolored appearance. Others experience pain, swelling, heaviness and cramping.” Dr. Corcoran adds that varicose veins are sometimes accompanied by tiny red veins known as spider veins.
What causes varicose veins?
“Varicose veins are caused by venous insufficiency,” remarks Dr. Corcoran.
Translation: weak or damaged valves inside veins let blood flow back into veins, rather than travel to the heart. Pooling blood in the veins causes them to twist and swell into varicose veins.
Who gets varicose veins?
The short answer: many people. “Venous disease is four times more common than artery disease,” says Dr. Corcoran, “and varicose veins is a prevalent venous condition.”
Risk factors for developing varicose veins include:
- Age
- Family history
- History of blood clots in the legs
- Hormones
- Standing or sitting for a long time
- Vein valve defects at birth
“The hormonal connection includes the menstrual cycle, pregnancy, birth control pills and hormone replacement therapy,” says Dr. Corcoran. “These hormones put women at risk specifically for deep vein thrombosis.”
If varicose veins are so common, why see a provider?
“Varicose veins can be a progressive condition,” cautions Dr. Corcoran. “When left untreated, symptoms can worsen and complications may arise, such as skin conditions, sores that don’t heal and deep vein thrombosis.” Dr. Corcoran reminds people that the earlier they receive a diagnosis and proper management from a vascular expert, the better the chances of staving off long-term problems.
Diagnosing And Treating Varicose Veins
How are varicose veins diagnosed?
“We use different imaging tests to diagnose varicose veins,” says Dr. Corcoran. “Imaging tests range from a specialized ultrasound that compares blood pressures in your ankle and arm to CT scans to venography.” Dr. Corcoran remarks that it’s important to have access to the full range of diagnostic capabilities. This helps ensure accurate diagnosis for the simplest and most complex conditions.
What treatment options are available for varicose veins?
“Although you can easily see varicose veins, they’re more than skin deep,” says Dr. Corcoran. “It’s not a matter of removing the varicose veins but rather treating their source.”
Modern treatments include both noninvasive and minimally invasive procedures. “One noninvasive treatment is sclerotherapy, in which we inject medication into affected veins,” notes Dr. Corcoran. “Minimally invasive procedures often take place inside the vein. Some of these leading-edge procedures use lasers, radio waves or stents.”
What kind of post-procedure downtime can I expect?
“Noninvasive and minimally invasive procedures deliver faster recovery times,” says Dr. Corcoran. “Most people can go back to their normal routine the next day. The interruption to your daily life is brief.”
What are treatment side effects?
Dr. Corcoran advises that treatment side effects are typically mild. “They usually include bruising or changes in skin color,” he says. “You’ll have a follow-up appointment to make sure you’re on the right track. But call your provider if you have any concerns beforehand.”
Do varicose and spider veins come back?
“Treatment is not always a ‘one and done’ situation,” Dr. Corcoran advises. “Varicose and spider veins can return, and you may need touch-up or annual procedures.”
What happens to the blood that previously went through varicose veins?
“Imagine your veins as service roads to a freeway,” Dr. Corcoran says. “We can close them off and still have flow to the bigger thoroughfares via alternate routes. Varicose veins are like wisdom teeth and tonsils. You don’t need them.”
Can you travel after a procedure?
“We recommend having a procedure after or well ahead of travel in which you’ll be seated for a long time,” recommends Dr. Corcoran. “If you travel after a procedure, give yourself a couple of weeks before you take that long road trip or plane ride.”
Dr. Corcoran also advises keeping the blood flowing when you do travel. “If you’re driving, pull over at rest stops at frequent intervals. If you’re flying, get up to use the restroom or pump your feet ten times every hour, as if you were stepping on a gas pedal.” Dr. Corcoran also reminds people to follow up after their procedure, as directed by their provider.
Are surgical procedures the only option for varicose veins?
“Depending on your situation, nonsurgical options may be right for you,” says Dr. Corcoran. “You can make lifestyle changes like walking, losing weight or eating a low-sodium diet.” Dr. Corcoran also suggests wearing compression stockings or socks. “You can find compression stockings at pharmacies, drugstores and online. With normal use, they typically last six months.”
What should I look for in a provider?
“You want an expert in the field,” says Dr. Corcoran. “See a vascular surgeon. They’re residency- and fellowship-trained in vascular medicine to diagnose, manage and treat simple and complex vascular disease.” Dr. Corcoran also suggests multispecialty groups for their comprehensive, whole-person care.
The bottom line? Don’t ignore your symptoms, and get the right care right away. See an expert to evaluate and treat your condition, whether it’s straightforward or an advanced form of vascular disease.
To find a vascular specialist at Henry Ford, visit henryford.com or call 1-800-436-7936.
Dr. Paul Corcoran is a vascular surgeon who sees patients at various Henry Ford Health locations, including Henry Ford Hospital in Detroit.