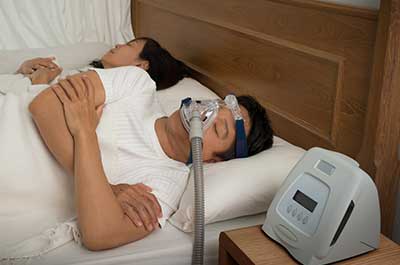
If your bed partner complains about your loud snoring—or you frequently wake yourself up with a snort—a condition called sleep apnea could be the culprit.
“Sleep apnea is a condition where you briefly and repeatedly stop breathing during sleep,” says Andrea Plawecki, M.D., an otolaryngologist and sleep medicine specialist at Henry Ford Health. Pauses can last anywhere from ten seconds to a few minutes and may occur more than 30 times an hour. This means your body and brain don’t get the oxygen they need to function properly. Not to mention the fact that you get far less restful sleep.
There are a few different types of sleep apnea:
- Obstructive sleep apnea, which occurs when throat muscles relax
- Central sleep apnea, which occurs when the brain doesn’t send proper signals to the muscles needed for breathing
- Complex, which occurs when you have a mix of obstructive and central sleep apnea
Left untreated, all three types of sleep apnea can lead to a myriad of health problems.
Here, Dr. Plawecki answers four frequently asked questions about sleep apnea.
1. Who is at risk for sleep apnea?
Depending upon which type of sleep apnea you have, the following factors may place you at risk:
- Being overweight or obese
- Having a narrow jaw or enlarged tonsils
- Taking certain medications, including narcotics, sedatives or tranquilizers
- Having a large neck -- 17 inches or more for men and 15 inches or more for women
- Smoking and drinking excessively
- Having nasal congestion
- Having high blood pressure, a previous stroke or other heart and brain problems
2. What are the complications?
Untreated sleep apnea can lead to a variety of issues from high blood pressure to heart failure. It may also contribute to depression, attention deficit hyperactivity disorder (ADHD) and – perhaps not surprisingly – poor performance at work due to fatigue. When your breathing becomes shallow, you often move out of deep sleep and into light sleep, resulting in sleep deprivation. You may be irritable, depressed and unable to stay awake at work – or worse, while driving.
3. What can you do before seeking medical assistance?
While sleep apnea is a potentially serious condition, it doesn’t always require medical intervention. In fact, some people can resolve the issue by losing weight and making other lifestyle adjustments. Avoid alcohol close to bedtime and steer clear of sedative medications, which can worsen sleep apnea. If you smoke, take steps to break the habit. Similarly, if you suffer from allergies, starting nasal sprays and allergy treatments can help keep your airways open. Even training yourself to sleep on your side instead of your back can help some breathe more easily.
4. What treatments are available?

Managing Sleep Apnea
Sleep apnea is a chronic condition that requires ongoing care and monitoring. The gold standard treatment for adults is a continuous positive airway pressure (CPAP) machine. This machine attaches to a small mask that fits over your nose and/or mouth and gently blows air into your throat to keep your airway open.
Other options include dental devices (which pull the jaw forward to open the airway), or surgery (either to remove obstructing tissue at the back of the throat, or to place a neurostimulator implant designed to treat sleep apnea.) Additional options may be available, depending on your unique circumstances. Talk to your doctor about your situation and what option might be right for you.
Unfortunately, sleep apnea often goes undetected. “Doctors can’t diagnose the condition during a standard office visit or with a simple blood test,” says Dr. Plawecki. “Instead, you have to wear monitoring devices or participate in a sleep study. It’s up to you to alert your doctor to poor sleep. If you experience shortness of breath, wake up choking and gasping for breath, or are excessively sleepy during the day, ask your doctor about sleep apnea."
That said, not everyone who has sleep apnea snores and not everyone who snores has sleep apnea. However, loud snoring is one indication of a possible obstruction, so if you or your partner snore loudly during sleep, it makes sense to get checked out.
Reviewed by Andrea Plawecki, M.D., an otolaryngologist and sleep medicine specialist who sees patients at Henry Ford Medical Center - Brownstown, Fairlane, New Center One, Plymouth and Templin.