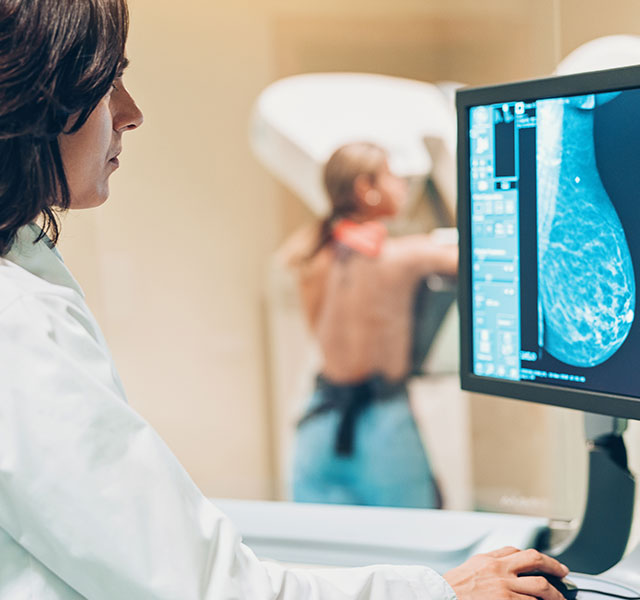
For years, there has been a lot of confusion over when and how often women should get screened for breast cancer. Multiple medical research organizations have offered differing guidelines and often left it up to individual providers to make the final call. Now there is a little more clarity.
The U.S. Preventative Services Task Force (USPSTF) recently updated their screening guidelines to align with other existing recommendations from accredited breast cancer research organizations. They now recommend that women with an average risk of breast cancer be screened every other year from ages 40 to 74. This is significant change from their 2016 recommendations that encouraged women to get screenings every other year from ages 50 to 74 and suggested that women talk with their doctor starting at age 40 to understand their individual cancer risk.
Here, Jessica Bensenhaver, M.D., a breast cancer surgeon at Henry Ford Health, explains the significance of this change and why beginning screenings at a younger age is so important:
Q: What do women need to know about these updated screening guidelines?
Dr. Bensenhaver: While the USPSTF is seen as a leader for recommendations regarding breast cancer screenings, there are many other organizations out there that have recommended mammograms starting at age 40 for average risk women for a long time. These guidelines have been based off clear data and backed by breast cancer-specific research. The science shows us that more women in their 40s are getting breast cancer, so starting screenings at 40 is essential. According to representatives from the USPSTF, by starting screenings at 40, there is a chance that up to 20% more lives are saved by early cancer detection.
Q: How have conflicting breast cancer screening recommendations impacted breast cancer numbers in recent years?
Dr. Bensenhaver: Ultimately, with multiple organizations having different recommendations, it has created a lot of confusion among patients. As a result, we saw a significant decrease in screenings following the 2016 USPSTF recommendations. The point of getting a mammogram is to identify breast cancer in its earliest stages when it is most treatable and with better outcomes. Any delays in screening can potentially put off a diagnosis, resulting in more advanced and complex cancer cases.
Q: What do these guidelines mean specifically for Black women?
Dr. Bensenhaver: Historically we’ve found that Black women were less likely to develop breast cancer, but if they did, it was at a younger age, was often a more aggressive, and with worse outcomes when compared to women of other backgrounds. Now, we’ve found that Black women are just as likely as any other women to be diagnosed with breast cancer, but there is still a huge discrepancy in their survival outcomes. Ultimately, these updated guidelines are a good thing – the earlier in life we start screening patients, the better our chances of reducing the breast cancer-related mortality rates of all women including Black women.

Q: What about patients that are high risk for breast cancer?
Dr. Bensenhaver: It is important to note that these recommendations are only for patients that are at an average risk for breast cancer. For high-risk cases, we hope to identify those patients as soon as possible (as early as 25 years old) so that we can institute a surveillance plan for them and potentially intervene to reduce their risk. However, patients often aren’t aware that they’re high risk until they’re told. To help identify these high-risk cases, at Henry Ford we offer risk assessment calculation at the time of their screening mammogram to quantify each patient's individual risk. This allows us to identify them and institute an appropriate surveillance plan as soon as possible.
Q: What should you do if you have questions or concerns about your breast cancer risk?
Dr. Bensenhaver: As providers, it is our job to help you understanding your personal risk of breast cancer. Talk with your physician or reach out to us to discuss what is best for you in terms of defining and potentially minimizing your risk. After assessing your risk, we can determine how best to procced from there. At a minimum, we recommend you should start breast cancer screenings at age 40. Additionally, I recommend annual screenings to my patients. It is much better to be proactive about your breast cancer risk and screening to minimize missing any early signs of cancer.
Reviewed by Dr. Jessica Bensenhaver, Director of the Breast Oncology Program at Henry Ford Health.