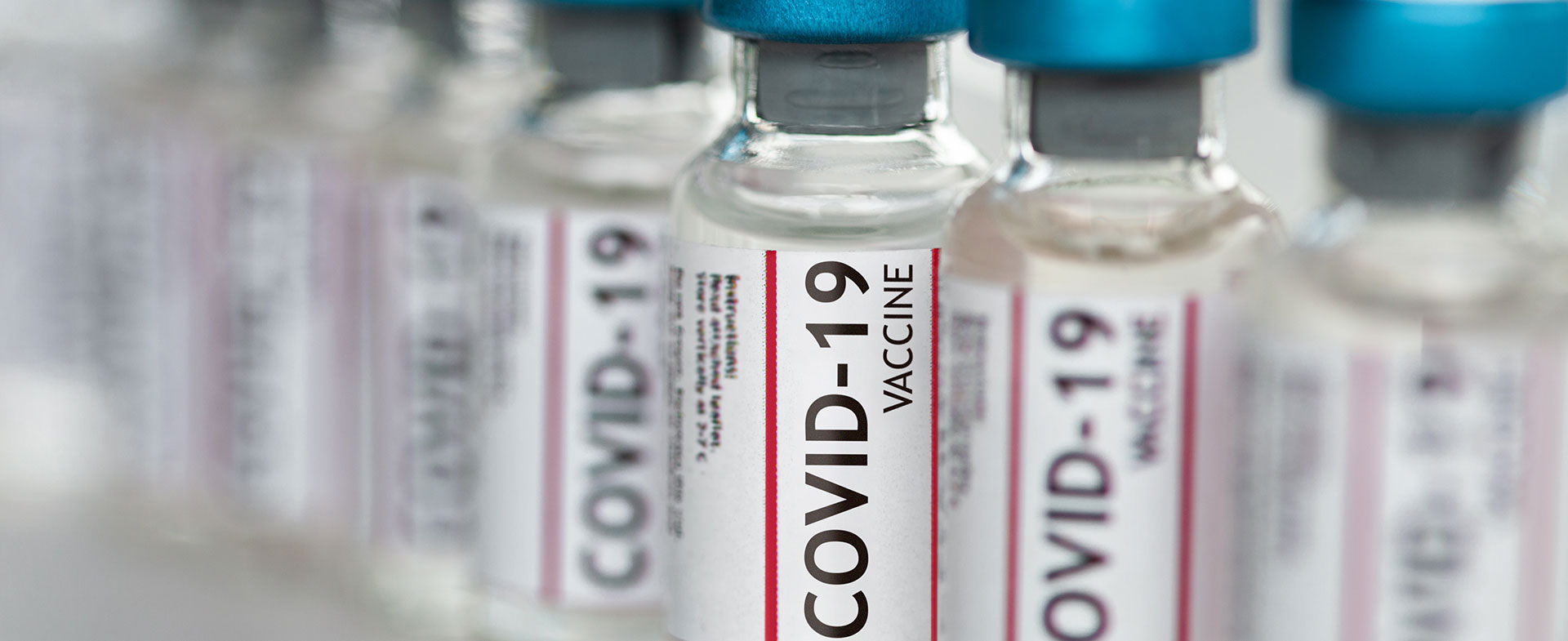
We are living through a historic time in scientific history: This is the fastest that scientists have ever developed a vaccine. Vaccines, of course, have eradicated tons of illnesses and have increased our life expectancy by many years.
In the past, it has taken years and years to develop vaccines that can be used in widespread populations, but with COVID-19, vaccines were developed in record time.
Using Scientific Advancements To Make The Vaccine
New research and technological advances allowed COVID-19 vaccines to be created faster than ever before. How did scientists and researchers do it?
“To know how they were able to fast-track these vaccines, you first have to know the steps it takes to create vaccines,” says Dennis Cunningham, M.D., medical director of infection control and prevention with Henry Ford Health. Here, he breaks the steps down:
1. Determine the genetic sequence of the virus. “30 years ago, it took years just to uncover the genetic sequence of a virus,” says Dr. Cunningham. “The longest part of the vaccine-making process, historically, has been this step: developing the molecule in the vaccine that is going to give you protection.” But thanks to scientific improvements, researchers quickly cracked COVID-19’s genetic code. Plus, COVID-19 has similarities to MERS and SARS, two other coronaviruses we’ve seen in humans. “We already had research from these two viruses, so we were able to use it to quicken this process,” he adds.
2. With this genetic material, develop a vaccine using one of a few different strategies:
- Inactivate the virus so that, while keeping its major components, it won't cause infection.
- Heavily weaken a strain of the vaccine so that it won't cause infection. Technically, it will still be alive, but it won't be strong enough to cause harm. This is called an attenuated vaccine, and it's how both the measles and some flu vaccines have been created.
- Pull out a specific component of the virus (i.e., parts of its genetic sequence, instead of the full genetic code) and use that as a vaccine, so that your body will recognize it and build up antibodies. “This is the method Pfizer and Moderna used to create their FDA-approved vaccines, which offer 95% protection against COVID-19," says Dr. Cunningham. "They both use a COVID-19 protein that attaches itself to our cells. After receiving the vaccine, our body becomes familiar with this protein and can build up antibodies to defend itself against contracting COVID-19.” This technology has been used to make cancer vaccines, which is a type of cancer treatment called immunotherapy, for more than 10 years.
3. Test the vaccine in 3 chronological phases of clinical trials:
- Begin with phase 1, which studies the vaccine in a small group of volunteers to see if it’s safe.
- Move on to phase 2, which tests the vaccine in a few hundred people to examine both safety and immune response to see whether it works.
- Finish with phase 3, which tests the vaccine in tens of thousands of people to examine safety and immune response.
Once these 3 phases have been successfully completed, a vaccine can be approved for widespread use.
“While the technology to develop these COVID-19 vaccines was fast, the clinical trials were not rushed at all,” says Dr. Cunningham. "These 3 phases of clinical trials were done carefully and properly, and the studies regarding safety and efficacy have been phenomenal—it’s a celebration of medicine and the scientific advances we’ve made over the years.”
Removing The Red Tape To Bring The Vaccine To Market
Along with scientific advancements, another reason why COVID-19 vaccines were created and approved so quickly is because the red tape was removed. Factors that usually hold up vaccine production and approval include:
- Recruiting scientists. It can take time to recruit enough scientists to work on vaccines. But the United States wasn’t at a shortage this time. Scientists were recruited from all around the world to aid COVID-19 vaccine research and development.
- Funding. Making a vaccine is extremely expensive. Usually, it can take years to raise the funds needed to develop a vaccine, but funding for COVID-19 vaccines came pouring in from U.S. agencies at the Department of Health and Human Services, along with private donors.
- Volunteers. Getting enough volunteers to participate in clinical trials is a huge hurdle, but given COVID-19’s notoriety, it didn’t take long for thousands of people to sign up and volunteer. Many were excited about the prospect of being vaccinated against the virus.
- Time lapses between clinical trials. Funding, volunteers, approvals: All of these factors can prevent a vaccine from moving swiftly through each phase of a clinical trial. With these barriers removed, phases were able to be completed back to back, without time wasted in between.
- FDA Approval. It can sometimes take years for the Food and Drug Administration (FDA) to approve a new medicine or vaccine. But in a state of emergency, the FDA can grant an Emergency Use Authorization (EUA) to provide more timely access to medical products. Because the COVID-19 vaccine clinical trials have shown such strong efficacy and safety, the FDA issued an EUA to approve the COVID-19 vaccine.
“Now, as we start rolling out the vaccines for public use, it’s up to us to get vaccinated,” says Dr. Cunningham. “Once they’re available for widespread public use in the coming months, we’ll see the end of this pandemic.”
For more information about the COVID-19 vaccines, visit henryford.com/coronavirus/vaccine-faqs.
To learn more about safety precautions at our facilities, ways to get care at Henry Ford, or for details on our response to COVID-19, ;visit henryford.com or call 1-800-436-7936.
Dennis Cunningham, M.D., M.H.A., is the medical director of infection control and prevention for Henry Ford Health.