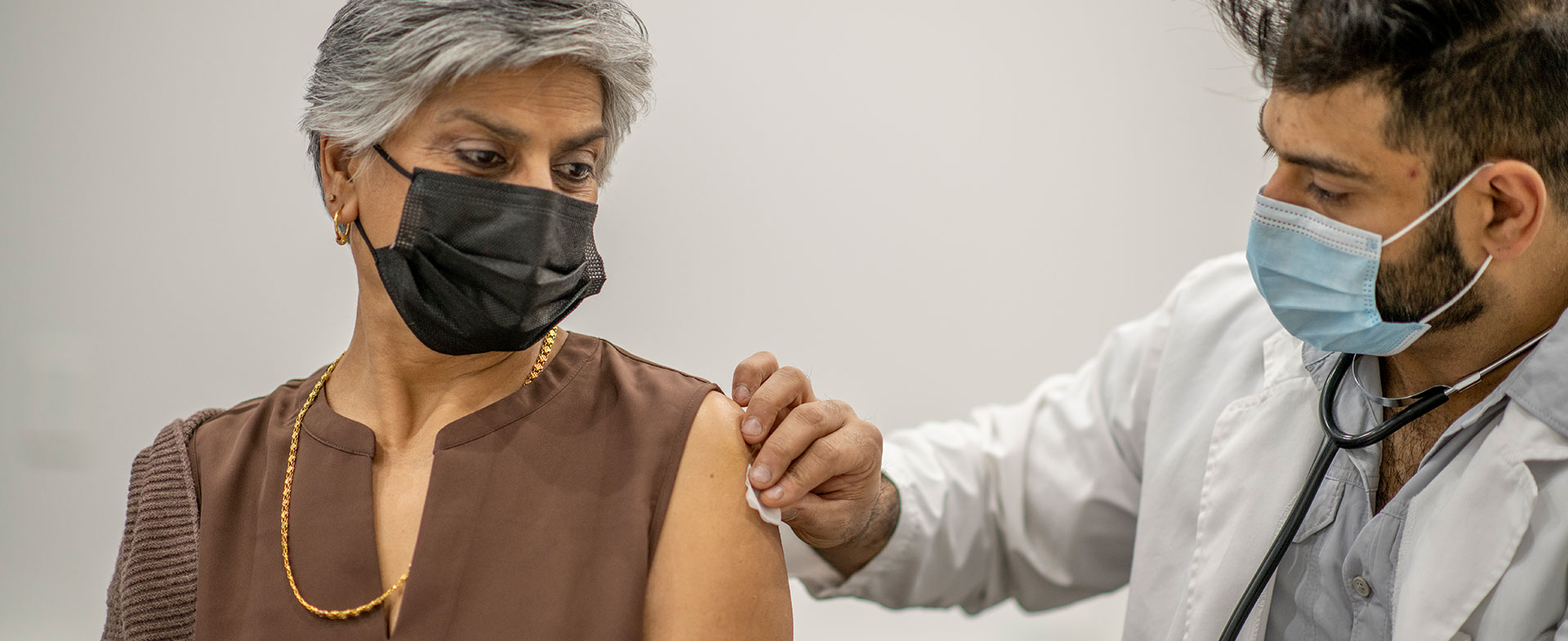
Johnson & Johnson’s COVID-19 vaccine recently received emergency use authorization from the Food and Drug Administration (FDA). This makes it the third COVID-19 vaccine available for public use. Pfizer’s vaccine was the first to be approved, followed by Moderna. In the race to end the pandemic, this is the news we’ve been waiting for.
“Johnson & Johnson expects to produce 20 million more doses by the end of March, and a total of 100 million doses by the end of June,” says Dennis Cunningham, M.D., MHA, medical director of infection control and prevention with Henry Ford Health. “That means the U.S. will have enough vaccine, when combined with the expected deliveries from Pfizer and Moderna, to vaccinate about 300 million people. That covers the entire adult population of the country.”
Just like the Pfizer and Moderna vaccines, Johnson & Johnson’s vaccine is safe and effective. It does not matter which vaccine you get—and you likely aren’t able to choose which one you do get. What matters is that you get the first vaccine that’s offered to you. The more people who are vaccinated, the sooner the threat of COVID-19 will decrease.
Here’s why all three vaccines—Pfizer, Moderna, and Johnson & Johnson—are beneficial tools to keep us safe and help us end the pandemic.
All of the vaccines are effective at preventing severe COVID-19 illness.
The Pfizer and Moderna vaccines are 95% and 94.1% effective at preventing illness, respectively, while the Johnson & Johnson vaccine is 72% effective at preventing moderate to severe illness, 86% effective at preventing severe illness and 100% effective at preventing death.
“While you may see that Johnson & Johnson’s efficacy isn’t quite as high as Pfizer or Moderna, it is difficult to compare the vaccines, because the clinical trials used different measurements and methods of data collection,” says Dr. Cunningham. “The Johnson & Johnson vaccine is still more effective than other vaccines, such as the flu vaccine,” he explains. “During the 2014-2015 flu season, with a flu shot that had 19% efficacy, the Centers for Disease Prevention and Control (CDC) estimated that flu vaccinations still prevented nearly 1.5 million cases of flu, more than 740,000 medical visits or hospitalizations, and almost 4,000 deaths.”
None of the vaccines contain live virus, so they cannot give you COVID-19.
Throughout history, some vaccines have been created using a live but weakened strain of a virus. While they are safe for healthy individuals, they may not be safe for those with compromised immune systems. None of the approved COVID-19 vaccines were created with live virus, however, so even those who are immunocompromised can get vaccinated.
Instead of weakened live virus, the Pfizer and Moderna vaccines use mRNA technology, while the Johnson & Johnson vaccine uses viral vector technology. Both types of vaccines are safe and effective:
- mRNA technology has been studied for decades and has been used in cancer treatment for 10 years. “These vaccines contain the instructions on how to create a small piece of the virus that causes COVID-19, called the spike protein,” says Dr. Cunningham. “Our body then makes this protein, recognizes it as foreign, and creates proteins (antibodies) to protect against it. That way, if you come into contact with COVID-19 in the future, your body will remember how to defend itself against contracting the virus.”
- Viral vector technology has already been used in Ebola vaccines, and is being studied for use in other vaccines. “A viral vector vaccine uses a harmless version of a virus to deliver important instructions to our cells,” says Dr. Cunningham. “For this vaccine, a virus – not the COVID-19 virus, but a different virus – enters a cell in the body and then use the cell’s machinery to produce COVID-19’s spike protein. Then, your immune system recognizes that spike protein doesn’t belong in our bodies. This tells our immune system to begin making antibodies and it activates other immune cells to fight off what it thinks is an infection. At the end of the process, our bodies are trained to protect us against the virus that causes COVID-19.”
Johnson & Johnson’s vaccine may make it easier for a larger number of people to get vaccinated.
For full vaccination, the Pfizer and Moderna vaccines require two shots, spaced three or four weeks apart, respectively. You are considered fully protected two weeks after your second dose. With Johnson & Johnson’s vaccine, only one shot is needed. You are considered fully protected two weeks after your single dose. This means that those who live in rural areas, or those who can’t easily return for a second appointment, can be vaccinated more easily.
Clinical trials are currently examining whether two doses of Johnson & Johnson's vaccine will increase effectiveness, but there is no information on mixing vaccines, so you should not do so.
“If your first shot is Pfizer, your second shot should also be Pfizer. Same goes for Moderna. And if you receive Johnson & Johnson, you shouldn’t receive any other shot,” says Dr. Cunningham. “The best vaccine is the one that’s offered to you.”
Visit henryford.com/vaccine for more answers to frequently asked COVID-19 vaccine questions.
To learn about safety precautions at our facilities, ways to get care at Henry Ford, or for details on our response to COVID-19, visit henryford.com or call 1-800-436-7936.
Dr. Dennis Cunningham is the medical director of infection control and prevention for Henry Ford Health.