Expert Care
Our radiation oncology team is known for developing the most advanced cancer therapies, including radiosurgery.
 Radiosurgery, also known at stereotactic body radiation therapy (SBRT), “removes” a tumor by delivering a high dose of radiation to a very precise area. This is a medical, not surgical treatment. Our Radiosurgery/Stereotactic Body Radiation Therapy (SBRT) program uses the most advanced radiosurgery technology, such as shaped-beam radiosurgery, image-guided radiosurgery, and intensity-modulated radiotherapy (IMRT). These technologies allow us to treat tumors anywhere in the brain, spine or body, including head and neck, lung, liver and pancreatic cancer.
Radiosurgery, also known at stereotactic body radiation therapy (SBRT), “removes” a tumor by delivering a high dose of radiation to a very precise area. This is a medical, not surgical treatment. Our Radiosurgery/Stereotactic Body Radiation Therapy (SBRT) program uses the most advanced radiosurgery technology, such as shaped-beam radiosurgery, image-guided radiosurgery, and intensity-modulated radiotherapy (IMRT). These technologies allow us to treat tumors anywhere in the brain, spine or body, including head and neck, lung, liver and pancreatic cancer.
Patients who undergo radiosurgery treatment in the morning can return to daily activities in the afternoon. Radiosurgery often requires a single dose of treatment but in some cases may require up to five sessions.
Our radiosurgery technology allows us to match the shape and size of the tumor from all angles, shape the radiation beam to deliver different levels of radiation intensity, and protect healthy tissue during radiation treatment. Two of the state-of-the-art systems we use in radiosurgery include:

Our radiation oncology team is known for developing the most advanced cancer therapies, including radiosurgery.
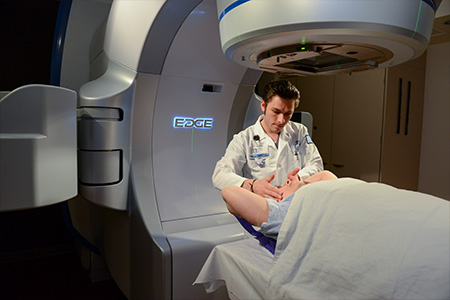
With the Edge radiosurgery system, tumors that are typically difficult to reach with traditional surgery can be targeted and treated with power and precision. The Edge system works by delivering large, targeted doses of radiation to obliterate cancer cells. To accurately deliver the recommended amount of radiation, the beam treats each part of the tumor from many different angles. Using precise beam sculpting and a real-time tracking system, we are able to deliver high radiation doses to destroy the tumor while minimizing exposure to surrounding healthy tissue. With an eye toward improving treatment ease and convenience, patients can expect a more comfortable experience because treatments with the Edge are typically completed within about 20 minutes, and most patients only need between one and five sessions.
Henry Ford radiosurgery specialists design a personalized radiosurgery treatment plan for every patient. In general, radiosurgery planning and treatment involves six main steps:
We use cookies to improve your website experience. By using this site, you agree to our Terms of Use. Read our Internet Privacy Statement to learn what information we collect and how we use it.