Expert Breast Cancer Care
We give patients access to the top surgeons and the most advanced science-based technologies and treatments.
There are many effective treatments available for breast cancer, and no two patients’ treatment plans will look exactly alike. We offer personalized treatment plans that are unique to your cancer type and stage, along with your priorities for care.
Your treatment plan likely will include one or more of these options:
Lymphedema, swelling in the arms and legs, is an unfortunate side effect that can occur after breast surgery or radiation therapy. We will work with you to reduce your risk of getting lymphedema and to manage its symptoms if it appears.
As part of your treatment plan, your care team may discuss your eligibility to participate in one or more clinical trials. These studies help researchers discover whether a new treatment or technique may be more effective than the current standard of care. Clinical trials may give you access to advanced therapies that are not yet available elsewhere.
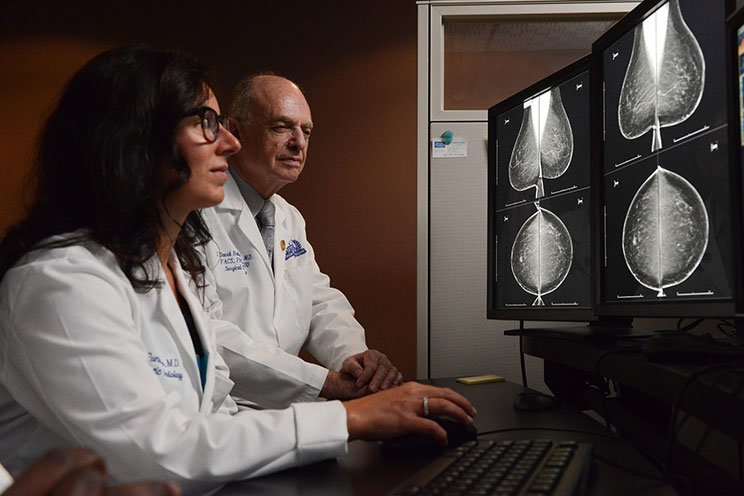
We give patients access to the top surgeons and the most advanced science-based technologies and treatments.

Our cancer team is here for you in-person, by phone and virtually for all your cancer care needs.
Mastectomy is required when a lumpectomy cannot be done. The most common reasons are if the tumor is too large or if the patient cannot receive the required radiation treatment.
Not all patients with breast cancer need chemotherapy. Receiving chemotherapy depends on the risk of cancer returning and the need to destroy undetected cancer cells. New tests can provide valuable information for chemotherapy decision-making. The tests can identify numerous genes in tumor cells and predict how breast cancer may progress in 10 years.
Radiation therapy is required to destroy any microscopic breast cancer cells in the:
We use cookies to improve your web experience. By using this site, you agree to our Terms of Use. Read our Internet Privacy Statement to learn what information we collect and how we use it.