Intraoperative MRI (iMRI) and Safer Brain Tumor Surgery
As part of your personalized treatment plan, your Hermelin Brain Tumor Center care team may recommend that you undergo surgery to remove a brain tumor. Any surgery comes with potential risks and can be a frightening experience. However, when it comes to your brain, this is even more true. Our minds help to shape who we are, and you may have concerns that brain surgery could affect your personality or ability to function.
Safer brain tumor surgery
Research has shown that removing more tumor tissue leads to a better surgical outcome. However, brain tumors are complex and may be located in areas of the brain where removal of healthy tissue could cause deficits. As part of the culture of safety at Henry Ford, the Hermelin Brain Tumor Center has worked to make brain tumor surgery as safe as possible, while helping to ensure the best possible outcome and highest quality of life.
Through innovative surgical technologies such as intraoperative MRI, we can more precisely identify your tumor and its relation to your vital brain centers, such as those that control speech, sensation, strength and vision.
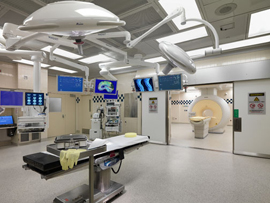
High-field intraoperative MRI (iMRI) suite
The high-field intraoperative MRI (iMRI) at Henry Ford Hospital is the first of its kind in Michigan. This advanced system uses a magnetic field and radio waves to provide real-time, high-resolution imagery of your brain’s anatomy during surgery. Some benefits of iMRI and related technologies include:
- Neuronavigation: This guidance system is linked to the images generated from the iMRI and is used routinely during surgery to determine the safest surgical route to remove the tumor.
- Compensate for movement: During surgery, the brain may shift, which can affect the precision of pre-surgical imaging. With real-time iMRI images your surgical team can adjust as necessary during surgery, based on the actual position of the tumor.
- Precision: With iMRI, your surgical team can better distinguish between the tumor and healthy brain tissue, and confirm that all of the imaged tumor has been removed, before completing the procedure.
- Mapping eloquent areas: For tumors embedded deep in the brain or near critical structures, iMRI also can be used in conjunction with functional MRI and fiber-tracking technology to visualize these eloquent areas.
- Awake craniotomies: In some cases, it helps to have you remain awake during the surgery. This way, your surgical team can ask you questions and perform some basic neurological tests to remove tumor tissue while helping to preserve vision, speech, strength and sensation. There are no pain receptors in the brain itself, so you will feel no pain during the surgery.
Ultimately, this intraoperative MRI technology allows for unprecedented surgical precision during brain surgery, ensuring the most complete tumor removal in the safest manner possible.
Innovative techniques using intraoperative MRI
Henry Ford also has used this technology to develop other innovative procedures for brain tumor surgery. For example, the Hermelin Brain Tumor Center team was the first in the United States to deliver a Trojan horse-like viral therapy to a brain tumor patient using intraoperative MRI guidance. This iMRI-guided viral therapy involves injecting into the tumor cavity a specifically engineered virus with the ability to attach to, enter and, ultimately, kill tumor cells without harming the neighboring normal brain cells. We have completed almost 1500 cases within the suite since its opening in 2011.
Safety research to help improve treatment outcomes and quality of life
Our team also is active in outcomes research and clinical trials, both of which help to ensure you receive the safest, most advanced surgical care while maintaining the highest quality of life.
.svg?iar=0&hash=F6049510E33E4E6D8196C26CCC0A64A4)

/hfh-logo-main--white.svg?iar=0&hash=ED491CBFADFB7670FAE94559C98D7798)