Our Expert Surgeons
Our prostate cancer team specializes in the most advanced treatments for prostate cancer.
 As a software engineer who works on hands-free driving projects, Anthony Bamgbose knows the importance of teamwork and cutting-edge technology. During his annual exam, a prostate-specific antigen (PSA) blood test was done to check for a protein made by prostate cells, possibly indicating prostate cancer.
As a software engineer who works on hands-free driving projects, Anthony Bamgbose knows the importance of teamwork and cutting-edge technology. During his annual exam, a prostate-specific antigen (PSA) blood test was done to check for a protein made by prostate cells, possibly indicating prostate cancer.
Concerns were raised, and his doctor requested further testing with a specialist. Soon, Anthony’s decision-making expertise would show up in his medical choices.
After a transrectal ultrasound and prostate biopsy at a hospital near his home, he was diagnosed with low-risk prostate cancer and surgery was scheduled. “I wasn’t comfortable,” says Anthony, a father of three who lives in Oakland Township. “I didn’t get enough information.
Knowing that two relatives had prostate cancer, he was driven to find facts and a second opinion.
“I went to the Henry Ford website, and they gave me more information about what was going on. I saw they were on the cutting edge of technology. The presentation was so great, I decided to contact Henry Ford right away,” says Anthony. “If I had gone to the other hospital, they may have been great, but they don’t tell you what they do. They say they provide service, but they don’t give you the details.”
At Henry Ford, Anthony was given the option of closely monitoring the cancer with prostate MRI imaging and a repeat biopsy with precision targeting of any abnormal areas on the MRI. Anthony felt reassured that his lower risk prostate cancer did not require immediate treatment and chose to watch and wait for at least a year.
Within six months he had a prostate MRI that showed a suspicious area, so a repeat biopsy was done. The biopsy was positive for clinically significant cancer, ranked as Gleason 7. He again elected for close monitoring over the next year. In June 2020, a repeat MRI and a targeted transperineal biopsy showed progression of the tumor and Anthony decided to schedule surgery to remove the prostate.
“Either his cancer had progressed to a higher-risk cancer or the MRI detected a higher-risk cancer that had already been there and was missed on his original non-targeted biopsy,” says Craig Rogers, M.D., chair of the Department of Urology. “We have made significant improvements in the safety and accuracy of our prostate biopsy technique at Henry Ford.”
Historically, a prostate biopsy involves needles randomly inserted through the rectum into the prostate to find cancer. “Instead of performing transrectal random biopsies, we have made a department commitment to perform prostate biopsies through a safer transperineal approach that reduces risk of infection and bleeding”, says Dr. Rogers. “We also offer an ‘executive biopsy,’ a one-stop process that provides fast-track results of MRI and targeted biopsy results in less than 48 hours, reducing anxiety and wait time”.
Soon after Anthony scheduled surgery, he received a call from Dr. Rogers, informing him of a new clinical trial at Henry Ford involving a targeted injection of a drug into his tumor. The goal was to shrink the tumor before surgery and to help completely remove cancer while sparing nerves.

“I believed the clinical trial drug would be helpful,” says Anthony. The drug had already been tried in a Phase I trial, and that gave me confidence. Also, I was confident I could stop the clinical trial at any time.”
Initially, his wife Ololade was concerned about any adverse effects. “She’s a nurse, and she did a lot of research about the medicine and side effects. Then she felt very comfortable.”
“We took a calculated risk, and we were very prayerful. That gave us confidence,” says Anthony in his home office cluttered with electronics.Accustomed to making important decisions, Anthony left Nigeria and came to the U.S. to attend college. He has already travelled to nearly 35 states. Ololade, also from Nigeria, came to the U.S. after their marriage.
As the first participant in the world in the Phase II NanoPac clinical trial offered only at Henry Ford, Anthony received three monthly, MRI-targeted injections of paclitaxel nanoparticles into the tumor.
“Every week I had a blood test to monitor for changes, and I was confident that the drug was going directly into the prostate tumor, not the blood stream,” says Anthony.Following the tumor injections, Dr. Rogers performed a robotic prostatectomy in February 2021 using the new single-port (SP) robotic system. The unique surgery required only one small abdominal incision for the multiple robotic instruments.
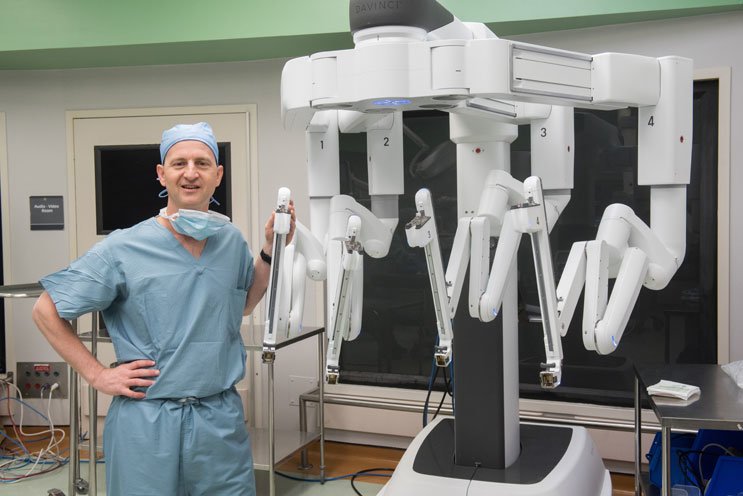
“All the robotic instruments go through a single incision and then branch out, similar to the arms of an octopus,” says Dr. Rogers, a fellowship-trained urologic oncologist specializing in robotic kidney and prostate surgery. He also has research interests in improving diagnostics and treatments for prostate cancer.
“The single-port system can help with an extra-peritoneal approach that avoids the usual technique of going through the abdominal cavity to get to the prostate. The smaller incision and less manipulation of bowel cavity can help make the surgery even less invasive than before,” says Dr. Rogers.
“After the surgery, I was able to move and walk gently the next day,” says Anthony. “And within a week, I was acting normally.”
Anthony’s prostate cancer was contained and his tests after surgery show that he is cancer free. “Anthony is a role model of the future of prostate cancer treatment,” says Dr. Rogers.
“Black men are more likely to have aggressive prostate cancer and more likely to die from it,” says Dr. Rogers. “It’s important to raise awareness about prostate cancer screening, particularly for men at higher risk. It is also important to raise awareness of improvements in the diagnosis and management of prostate cancer.
“Those improvements include prostate monitoring, imaging, safer and more precise targeted biopsies, along with minimally invasive treatments and the latest clinical trials. Anthony was an example because he experienced the entire spectrum of innovations in all of these areas.”
“I’m glad I got a second opinion at Henry Ford,” says Anthony who continues to monitor his PSA levels. “I advise other patients to talk to their doctors, do their own research and be prayerful. You have to feel good about doing a clinical trial.”
Our prostate cancer team specializes in the most advanced treatments for prostate cancer.
We use cookies to improve your website experience. By using this site, you agree to our Terms of Use. Read our Internet Privacy Statement to learn what information we collect and how we use it.