A Good Life After Complicated, Awake Craniotomy

Janae Nelson, a 29-year-old speech and language pathologist, had a lot going for her. She was planning her wedding and a honeymoon to Scotland and Ireland when COVID hit. Her recovery was slow, and some symptoms were odd. Instead of a trip to Europe, all roads would lead her to Henry Ford and the neurosurgery team that would save her life.
Before COVID, Janae loved to work with her patients, hike, travel, play games, and mostly – visit with family and friends. But COVID wiped her out. Exhausted and experiencing problems in her lungs, heart and eyes, Janae would sometimes wake up feeling as if one side of her head were asleep. The wedding was rescheduled, the guest list shrunk, and the honeymoon redirected to the Upper Peninsula.
Symptoms continued, but the medical tests came back negative. “With the attention deficits and flashing lights, I believed I needed to see a neurologist,” says Janae. One month later, she walked into a clinic for an MRI and EEG. Before she went home, a nurse asked her to talk with the neurologist. “That’s when he told me I had a brain tumor,” says Janae.

The doctor explained if he had a son or daughter, he would recommend Jack Rock, M.D. at Henry Ford. Soon Janae’s friends were recommending the same hospital. “All roads were pointing me to Henry Ford,” says Janae.
“We get a lot of referrals because a lot of practices around the state don’t want to do a craniotomy while the patient is awake. Yet, most people would acknowledge that it is the safest for the patient in a situation like this one,” says Dr. Rock.
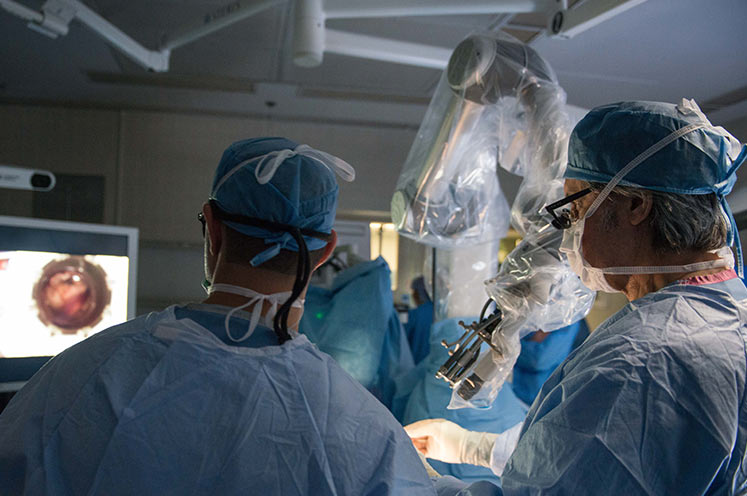
Awake Craniotomy
Cancer Support Services
We offer a variety of support programs make sure the whole patient is being taken care of during cancer treatment, including emotional, physical and spiritual services.
Talking during surgery
 Within three days, Janae and her husband Torri were sitting in Dr. Rock’s office. “When I heard I was getting an awake craniotomy, the speech pathologist part of me said ‘Oh, that’s so cool.’ Then I realized I shouldn’t be excited,” laughs Janae.
Within three days, Janae and her husband Torri were sitting in Dr. Rock’s office. “When I heard I was getting an awake craniotomy, the speech pathologist part of me said ‘Oh, that’s so cool.’ Then I realized I shouldn’t be excited,” laughs Janae.
While removing the uncommon grade 3, anaplastic astrocytoma, Dr. Rock worked to protect the speech and language center of Janae’s brain. “I was awake and speech-therapizing myself during the surgery, even though there were two speech therapists in the operating room,” says Janae.
While her brain was still open, Janae was wheeled to another area of the operating room and an MRI (https://www.henryford.com/services/brain-tumors/treatments/surgery/imri) was done to identify any remaining tumor cells.
“The tumor was near her speech center, which was a complicating factor. We removed the majority of the tumor, but there’s always a residual – that’s why you get chemotherapy and radiation therapy after surgery,” says Dr. Rock. “You can’t tell in the operating room whether you’re dealing with tumor alone or a tumor mixed with normal neurons. By taking out as much as you can, you can improve the prognosis.”
To determine precise chemotherapy and radiotherapy, neuro-oncologist James Snyder, M.D. ordered a complete genome analysis of the tumor specimens. “She had some molecular features that are encouraging and usually associated with a little better prognosis,” says Dr. Rock.
Mira Shah, M.D., a radiation oncologist specialist did radiation mapping and her team customized a protective mask. Janae wanted to preserve her fertility, so her eggs were retrieved, embryos were created and finally stored. Then she was ready to start six weeks of chemotherapy and radiotherapy, followed by six cycles of a higher dose chemotherapy.
Recovery from side effects
“The exhaustion was unlike anything I’d ever felt,” says Janae who experienced persistent nausea. “Following surgery, I had aphasia. People had to figure out what I was saying, and the overall stress impacted everyone.”
“In the operating room she was speaking nicely, but then the brain swells as a reaction to the operation,” says Dr. Rock. “It takes a couple weeks before that improves, and during that time patients have worse speech, which can be terrifying.”
“I use a lot of communication strategies I’ve used with my patients. Within a few months, I was conversational,” says Janae. “My husband was my rock, and our families were extremely helpful.”
“After having COVID and cancer treatment, I could only walk for 10 minutes,” says Janae. “I credit Henry Ford’s ExCITE program for getting me back in shape.” She also received speech therapy, acupuncture and cognitive therapy to help relieve anxiety. Currently, Janae does weekly virtual exercise sessions.
Since the surgery, Janae and Torri have moved to Midland, near their parents. “We have tons of happy moments. We continue to live life and persevere. We try to stay positive,” she says.
Serious but hopeful
 “I’m more spontaneous now, I’m not waiting to live life anymore,” she says. “I have so many blessings, and I don’t stress about the little things. But sometimes the gravity of the situation hits me. As a speech and language pathologist and now a patient, I know the symptoms I could face. But I don’t know what the future holds. I remain so hopeful,” says Janae.
“I’m more spontaneous now, I’m not waiting to live life anymore,” she says. “I have so many blessings, and I don’t stress about the little things. But sometimes the gravity of the situation hits me. As a speech and language pathologist and now a patient, I know the symptoms I could face. But I don’t know what the future holds. I remain so hopeful,” says Janae.
“Henry Ford saved my life. I trusted them implicitly,” says Janae. “They were incredibly thorough and knowledgeable. They were compassionate and took time to answer all my questions. They were very honest about this serious diagnosis, but they filled me with hope about the future and medical advancements. These are competent people who want to help, and they have the research and clinical trials to back it up.”
Some lessons learned from her parents have been helpful: Take one step at a time, be kind and be generous, says Janae. “I consider myself an empathetic person, but this has created even more empathy in me.”
Janae’s advice
Be careful if you do internet searches. Medical advances are always being made, and every patient’s story is different. There’s no way to know accurate prognostic factors.
Allow yourself to grieve, but always try to maintain gratitude and a positive attitude. Look for the silver lining every day. And try to keep your physical strength even though you feel bad. Don’t hesitate to get therapy and encourage your caregivers to do the same. Most of all – enjoy time with your loved ones.
The future?
“I want to start a family next year,” says Janae. “I want to focus on happiness and live my best life.”
.svg?iar=0&hash=F6049510E33E4E6D8196C26CCC0A64A4)

/hfh-logo-main--white.svg?iar=0&hash=ED491CBFADFB7670FAE94559C98D7798)
