Clinical Trials Explained
What is a clinical trial? Am I a good candidate for a clinical trial? These questions and more are answered by Henry Ford clinical trials experts.
In addition to standard cancer treatments, some patients also have the chance to participate in clinical trials. These studies allow cancer experts to test new methods of diagnosing and treating cancer. Clinical trials give you access to treatment not yet available to the general public as well as the chance to help us advance cancer research and treatment for future patients.
For example, we were one of just six hospitals to participate in a clinical trial for the revolutionary NanoKnife treatment for pancreatic cancer. This treatment has been shown to double the survival time of advanced pancreatic cancer patients compared with traditional methods. The Henry Ford Clinical Trials Office is one of the most comprehensive resources of its kind in the nation.
What is a clinical trial? Am I a good candidate for a clinical trial? These questions and more are answered by Henry Ford clinical trials experts.

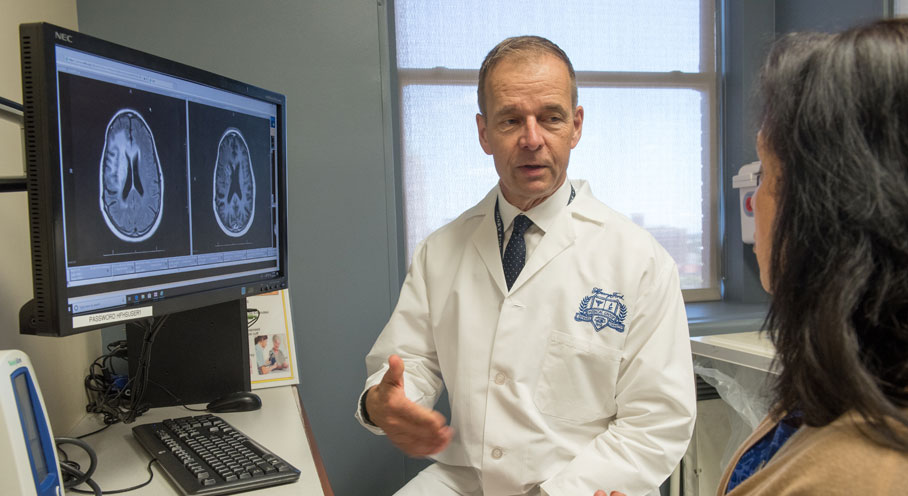
The adaptive clinical trial for brain cancer, GBM AGILE is a major step forward for Precision Medicine.
We were selected as the first-ever to activate two new treatments for glioblastoma care.
Treatments are carefully studied by medical experts in a laboratory to determine safety and effectiveness before they advance to the clinical trial stage. Before you participate in a clinical trial, we’ll guide you through the treatment methods as well as the trial’s potential benefits and risks. Participating in clinical trials is voluntary.
The Henry Ford Clinical Trials Office is one of the most comprehensive resources of its kind in the nation. For example, we were one of just six hospitals to participate in a clinical trial for the revolutionary NanoKnife treatment for pancreatic cancer. This treatment has been shown to double the survival time of advanced pancreatic cancer patients compared with traditional methods.
Henry Ford Health is also the first in the country to perform a clinical trial procedure using the CG-100™ intraluminal device, which is designed to help patients undergoing gastrointestinal resection from colorectal cancer treatment. The CG-100™ device is temporarily inserted into the gastrointestinal tract to reduce the need for an ostomy bag, eliminating additional surgery and recovery for the patient. Henry Ford is the only site in Michigan, and one of a select few throughout the country, currently enrolling colorectal cancer patients in this clinical trial.
Through a process called informed consent, you will learn about a study's treatments and tests, and possible benefits and risks, before deciding whether or not to participate.
Every study has guidelines for who can participate. There are many factors that may be taken into account, including type of disease, age, and gender. Ask your doctor if you are eligible to participate in any of our current cancer clinical trials. The U.S. National Institutes of Health also maintains a current list of national clinical trials online.
Health insurance plans and managed care providers don’t always cover all patient care costs in a clinical trial. Coverage varies by plan and by study.
Ask a doctor, nurse or social worker from the study to help determine in advance what costs are covered. Research costs -- such as the study drug or treatment, tests, and doctor appointments -- may be covered by the study sponsor.
Most clinical trials progress in an orderly series of steps, called phases. This allows researchers to ask and answer questions to protect the patient and result in reliable information about the drug or treatment being tested. Clinical trials usually are classified into one of four phases:
We use cookies to improve your website experience. By using this site, you agree to our Terms of Use. Read our Internet Privacy Statement to learn what information we collect and how we use it.